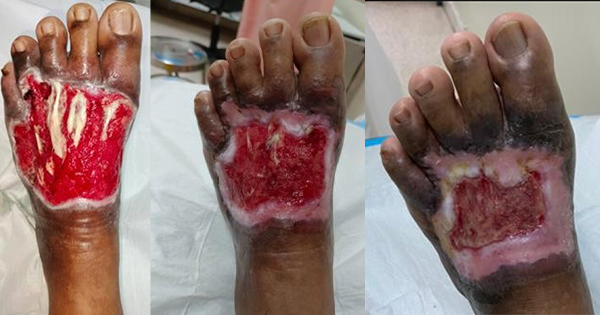
Patients with wounds due to an underlying autoimmune disorder present a unique challenge for wound care professionals. Firstly, the complexity of the wound and its aetiology requires a multidisciplinary approach. Secondly, the use of immunosuppressive therapy — essential to control the systemic immune response — increases the risk of infection and slows down the normal wound healing processes. Here we present two case reports on autoimmune disease-related wounds in two female patients. The first case involved a young adult with a systemic lupus erythematosus (SLE) who had a wound over the left gaiter region for more than a year and had been treated with multiple hydrogel dressings without showing improvement. The second case is an elderly patient who developed multiple necrotic wounds over her bilateral lower limbs. She had been treated with conventional dressings for several months but once her biopsy results revealed that she had pyoderma gangrenosum (PG), was switched to a polymeric membrane dressing (PMD). Both patients recovered well with no recurrence after wound re-epithelization.