Autolytic debridement is the lysis or breakdown, of damaged tissue in a wound that occurs as a result of the body’s natural defence mechanism using enzymes that breakdown specific components of body tissue or cells, such as protein, fibrin and collagen (Bryant and Nix, 2015). Hydrogel dressings that provides optimal conditions for the body’s natural enzymes to initiate autolytic wound debridement. (Bluestein and Javaheri, 2008). Hydrogels are complex three-dimensional (3D) structures composed of hydrophilic polymers that are interconnected through physical or chemical crosslinking. These hydrophilic structures exhibit a remarkable capacity to absorb exudates from wounds and facilitate the flow of oxygen, hence promoting the healing process (Kumar and Jaiswal, 2016).
Here we examine the use of a hydrogel formulation containing carboxymethylcellulose (CMC)-alginate, glycerol, lactate and filtered water on wound bed preparation.
Methodology
Data was compiled retrospectively. Details regarding history, physical examination, investigation, diagnosis and intervention were taken from the patients’ medical records from their twice weekly outpatient follow-up, at the Wound Care Clinic. Wounds assessments were performed at each visit, including the measurement of wound length and width using a disposable ruler.
Case summary
Case 1
A 42-year-old female with underlying diabetes mellitus, hypertension and a history of ray amputation of the second, third and fourth toes 6 years ago. She had an infection over her left leg that was complicated by septic arthritis. She underwent an arthrotomy and washout of her left ankle, and wound debridement of her left leg. Her wound was managed by Orthopedic Team for six weeks before referal to the wound clinic.
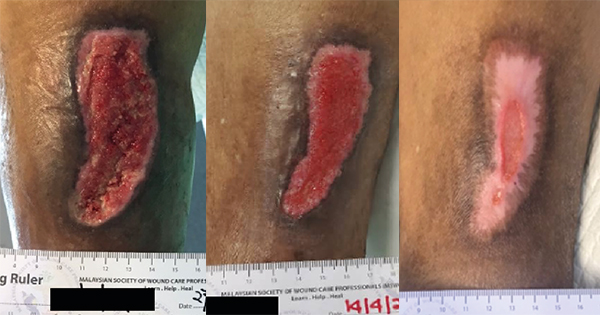
There were three separate wounds located at the lateral thigh (Case 1A), ankle (Case 1B), and dorsum of the left foot (Case 1C). Examination on day 1 showed a dry and necrotic tendon over the wound at the lateral left leg and left ankle, which subsequently underwent sharp debridement. Silver hydrofiber dressing together with CMC-alginate hyrodgel were applied over the wound bed for two weeks. After two weeks, silver hydrofiber dressing was stopped and same CMC-alginate hyrodgel was used. The wound size of the left lateral thigh, left ankle and the dorsum of the left foot reduced by 16%, 12.5% and 26.40%, respectively by day 16 as shown in Case 1A–C. The wound at her left ankle healed by day 44 while the other two wounds reduced in size and had good granulation tissue.
Case 2
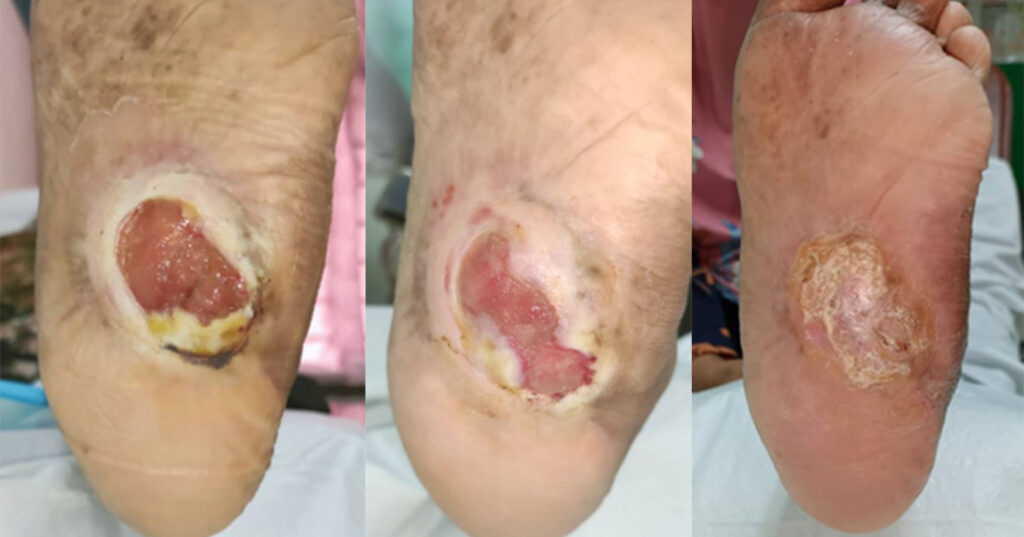
A 56-year-old female with underlying diabetes mellitus, hypertension, ischaemic heart disease, and end-stage renal failure was referred by the primary care team for a left diabetic foot ulcer with underlying Charcot’s arthropathy and midfoot collapse. The wound was initially observed three years ago and progressively increased in size and was associated with pain, especially upon weight bearingg. She was previously treated with daily superoxidized solution dressings at her nearest clinic. Case 2 illustrates the wound progression when treated with CMC-alginate hyrodgel. The wound size reduced by 56% at day 48 and 79% at day 89 with good granulation tissue formation. The patients complied with wearing offloading shoes and the wound had subsequently healed by day 173.
Discussion
In the first case, sharp debridement was done to remove the unhealthy tendon and tissue followed by the a combination of a hydrofiber silver dressing and CMC-alginate hydrogel was applied over the wound bed for the initial two-week period. The hydrofiber silver dressing functions as a localised antibacterial agent and an absorbent dressing. As the wound and clinical signs improved, the dressings were changed to CMC-alginate hydrogel alone. In the second case, CMC-alginate hydrogel was used from the initial visit until the wound was closed.
Hydrogel aids to promote granulation tissue development and maintain hydration of the exposed bone or tendon. Carboxymethylcellulose exhibit a strong affinity to water rendering CMC hydrogels highly absorbable to wound exudate. (Naseri-Nosar and Ziora, 2018). Additionally, the hydrophilic nature of CMC facilitates the maintenance of a moist wound environment that promotes the proliferation and migration of fibroblasts and keratinocyte cells. In addition, the moisture may potentially enhance the cell’s proliferation, enzyme activation, growth factor secretion and hormones regulation (Kanikireddy et al, 2020).
Alginate is a water-soluble, high-swelling polysaccharide derived from the cell walls of brown algae and certain bacteria species, such as Pseudomonas or Azotobacter (Mushollaeni, 2011). Alginate has a remarkable swelling capacity where it can expand to 20 times its own weight and jellify in wound environments, thus providing moisture and stimulating epidermis regeneration (Hong et al, 2008). Glycerol is added to increase alginate water solubility, swelling degree and flexibility (Da Silva et al, 2016). These dual actions of alginate and CMC in this particular hydrogel are effective in maintaining a moisture-balanced wound environment.
Limitations
This is a small sample of case studies and further prospective trials are required in the future.
Conclusion
In this case study, both cases responded well to CMC-alginate hydrogel. Selecting an appropriate dressing based on a thorough evaluation of the wound is a pivotal aspect of effective wound treatment, since it facilitates expedited wound healing.