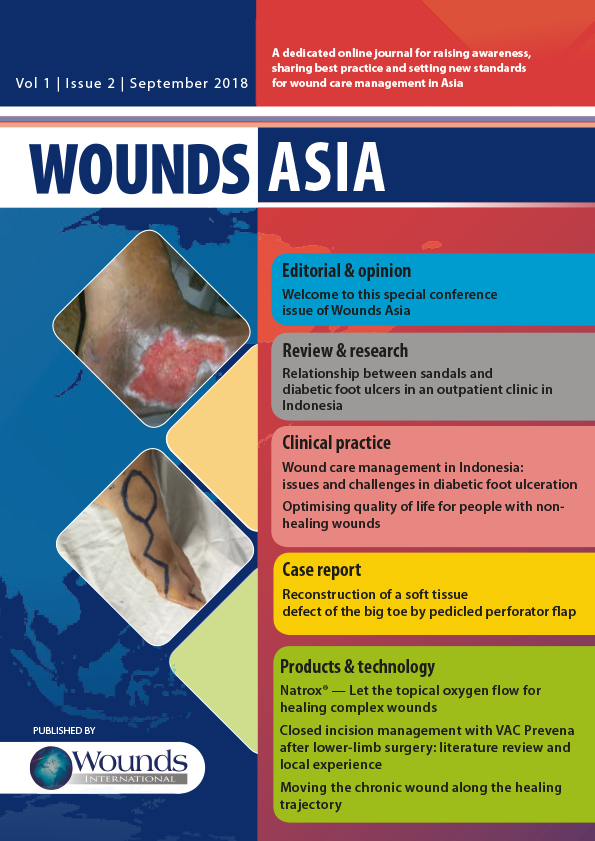
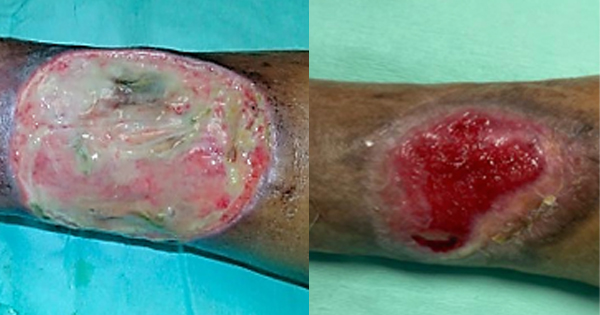
Patients who undergo vascular surgical procedures are often elderly and have concomitant diabetes mellitus and ischaemic heart disease. In our population, a substantial proportion also have end-stage renal failure. All of these factors contribute to poor wound healing and a propensity for wound breakdown and surgical site infection (SSI) (Cheadle, 2006; Kalish et al, 2014; Turtiainen et al, 2014). Vascular surgical incisions are usually extremely long (e.g. long saphenous vein harvest for femoral–popliteal or popliteal–distal bypass) or sited in dirty areas (e.g. the groin) or on the distal aspects of the lower extremity where vascularity is most tenuous (e.g. the foot).
The reported incidence of SSI in the groin after vascular surgery ranges from 3% to 44% (Matatov et al, 2013; Pledger et al, 2018). Matatov and colleagues (2013) found a 30% postoperative infection rate in patients treated with conventional dressings, while Pledger et al (2018) reported a 17% local infection rate and wound healing complications in 45% of patients receiving conventional therapy following vascular surgery. The rate of leg wound complications after long saphenous vein harvest is somewhat less, ranging from 1% to 24% of cases (L’Ecuyer et al, 1996; Slaughter et al, 1993; Gaballah et al, 2013). One series, however, reported complications in 32.6% of patients (Fowler et al, 2005).
We report the results of a literature review assessing the efficacy of negative pressure wound therapy (NPWT) in closed incision management following surgery. The rates of SSI are compared to conventional therapies. We then provide details of five cases where we have used vacuum-assisted closure (VAC) with Prevena™ to prevent SSI.